Hvala! Vaš zahtjev je zaprimljen. Uskoro ćemo Vas kontaktirati.
Specijalna bolnica za oftalmologiju Svjetlost
- E-mail: info@svjetlost.hr
- Tel: +385 1 777 5656

Film Legacy
Povodom 25. godišnjice Klinike Svjetlost
Naši liječnici
Klinika Svjetlost ima više od 80 zaposlenih oftalmologa, 2 anesteziologa, 4 profesora oftalmologije, 2 docenta, 3 primarijusa i preko 250 zaposlenih djelatnika.
saznajte više
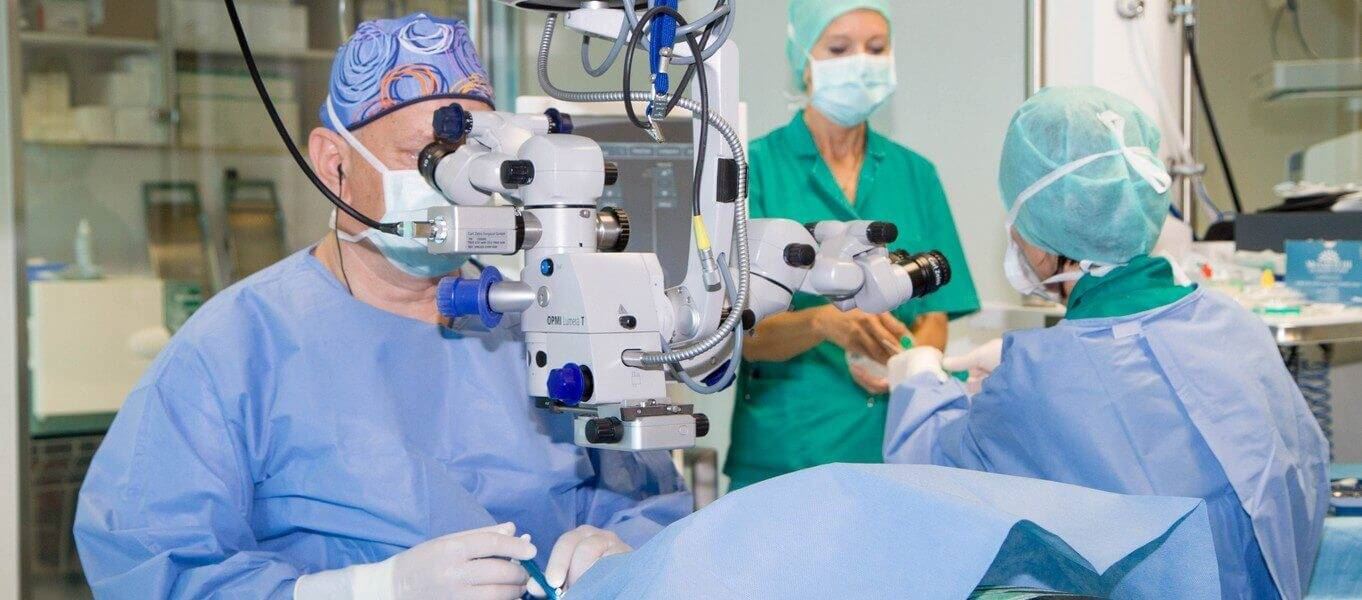
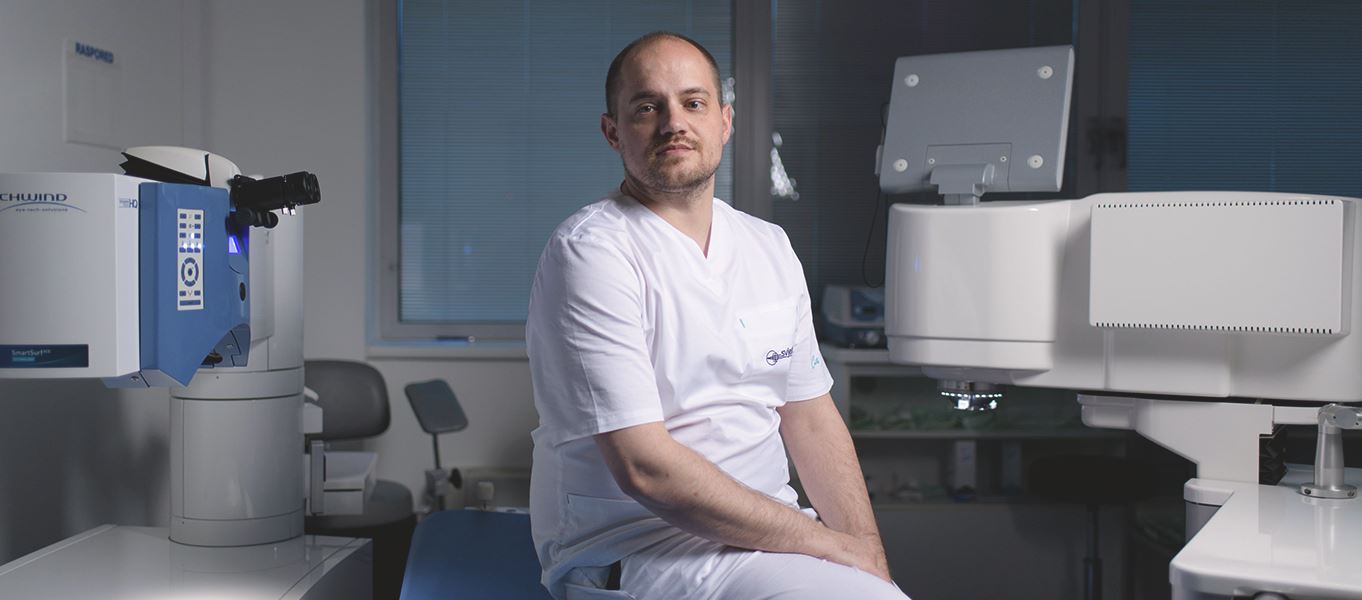
Vrhunska tehnologija
Bolnica raspolaže sa 6 vrhunski opremljenih operacijskih dvorana u kojima je moguće zbrinuti sve bolesti oka koje zahtijevaju kirurško liječenje – lasersko skidanje dioptrije, ultrazvučna i laserska operacija katarakte, operacije na stražnjem dijelu oka kod bolesti uzrokovanih dijabetesom, bolestima žute pjege ili degenerativnim promjenama.
saznajte više
25 godina
iskustva
80
stalno zaposlenih oftalmologa
250.000
operacija oka
800.000
pacijenata
5 centara
oftalmološke izvrsnosti

ZAGREB
SPLIT
SARAJEVO
BUDVA
SKOPJE
Rezervirajte termin
Klinika Svjetlost
- e-mail: info@svjetlost.hr
- Telefon: +385 1 777 5656
- Fax: +385 1 777 5600
- Heinzelova 39, 10 000 Zagreb
- Hrvatska
- e-mail: split@svjetlost.hr
- Telefon: +385 21 783 050
- Fax: +385 21 783 068
- Borisa Papandopula 8b, 21 000 Split
- Hrvatska
- e-mail: info@svjetlost-banjaluka.ba
- Telefon: +387 51 439 592
- Fax: +387 51 439 588
- Bulevar srpske vojske 17, 78 000 Banja Luka
- BiH
- e-mail: info@svjetlost-sarajevo.ba
- Telefon: +387 33 762 772
- Fax: +387 33 762 771
- Dr. Mustafe Pintola 23, 71 000 Sarajevo
- BiH
- e-mail: info@svjetlost.hr
- Telefon: +385 1 777 5656
- Fax: +385 1 777 5600
- Heinzelova 39, 10 000 Zagreb
- Hrvatska
- e-mail: info@svjetlostbudva.me
- Telefon: +382 33 451 121
- 22. Novembra 7, 85310 Budva
- Crna Gora